
Infant Meningitis and Your Baby’s Health
Meningitis is inflammation of the meninges (the three membranes) that line the brain and spinal cord. Newborn babies are at a much higher risk of developing meningitis than any other age group, as their immune system is weaker and more susceptible to viruses and illnesses. Meningitis can develop from bacteria, viruses or fungus that infect their body and travel to the bloodstream.
Before the pneumococcal vaccine became standard, around 10 out of every 100,000 babies under one year old got meningitis. Now, the rate is much less – around 8 out of every 100,000 babies get some form. In neonates, or babies less than 28 days old, meningitis affects around 0.1 to 0.4 out of every 1,000 live births. While infant meningitis is a serious medical condition, around 90% of babies who get it survive. Unfortunately, 20-50% of survivors do have long-term health problems, including vision problems and learning difficulties.
What is Meningitis?
Meningitis happens when a viral or bacterial infection spreads to the spinal fluid and spinal cord. Neisseria meningitidis and Streptococcus pneumoniae are forms of bacterial meningitis, and are considered much more dangerous than viral meningitis. Viral meningitis is still the most common type, as most bacterial forms are controlled with vaccines. Fungal meningitis is also quite rare.
Whereas viral meningitis can typically resolve on its own without extensive treatment in older children or adults, infant meningitis should be treated immediately. Bacterial meningitis is a serious illness that can lead to brain damage, hearing loss, and even death. Although it was more common prior to the 1990s, Haemophilus influenzae type b is another cause of bacterial meningitis.
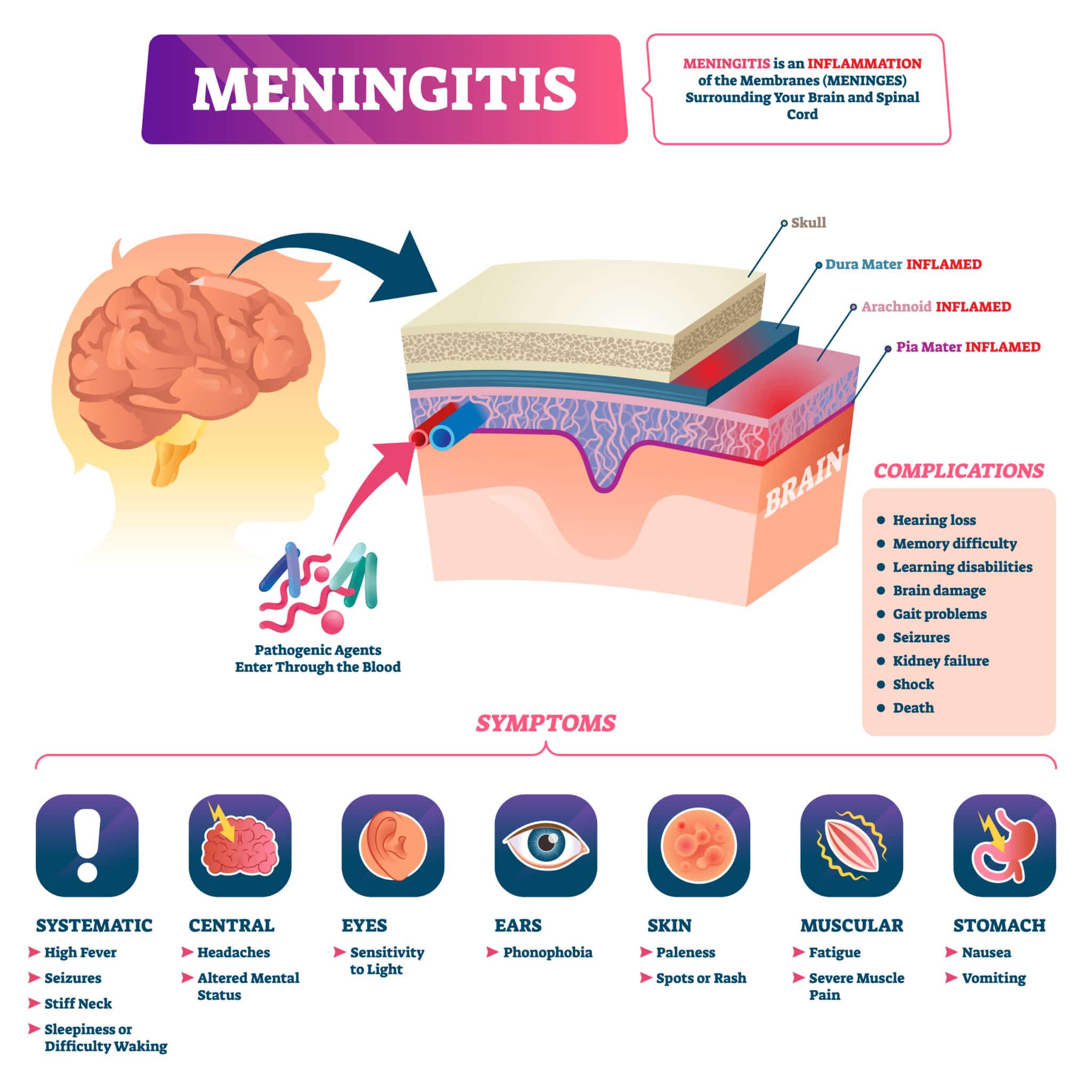
What Causes Meningitis?
Physicians test pregnant women for various viruses and bacteria, such as HIV, syphilis, herpes simplex virus and Group B strep. They are not, however, tested for all forms of bacteria, viruses or fungi that can cause meningitis.
Viral Causes
Some of the most common viral causes of meningitis include:
Non-polio enteroviruses
Most cases of meningitis in the U.S. are caused by enteroviruses. Enteroviruses include many types of infections, including the common cold. Each year, many people get enteroviruses, but very few of them will develop meningitis. For infants, these viruses spread when the baby comes in contact with oral secretions (cough, sneeze, etc.) or fecal matter.
Influenza
The influenza, or flu, virus can also develop into meningitis. Flu viruses are spread from oral secretions of someone who is infected. This is why people with the flu are urged to cover their coughs and sneezes.
Measles and Mumps
Measles and mumps are fairly rare, but very contagious viruses. Meningitis is a rare complication of these two viruses, which are spread from oral secretions, such as coughing or sneezing.
Varicella
Varicella is one of the viruses that can lead to severe meningitis. It is the virus that causes chickenpox. It is very contagious and is easily spread through person-to-person contact.
Herpes Simplex Virus
Herpes simplex virus is generally transmitted from the mother to the baby during birth. Also called HSV, this virus can manifest on different parts of the body. There are two strains:
- HSV-1: Causes oral herpes. People with HSV-1 may have cold sores or fever blisters on their face or mouth.
- HSV-2: Causes genital herpes. This is the type that causes outbreaks of genital herpes. It can easily be spread to a baby during delivery, especially if the mother is having an outbreak.
West Nile Virus
West Nile Virus, or WNV, is the most common cause of mosquito-borne illness in the U.S. It is spread when an infected mosquito bites someone. There are currently no vaccines for WNV or treatments. Most people with WNV experience no symptoms. Around 1 in 5 people have flu-like symptoms. Only 1 in 150 people infected have serious illness.
Bacterial Causes
Some of the most common bacterial causes of meningitis include:
Group B Streptococcus
Group B Streptococcus (Group B Strep) is a bacterial that affects around 15-35% of women. Most women do not have symptoms, even though the bacteria lives in the genital area. GBS is not a sexually transmitted disease and doctors are unsure of exactly how it is transmitted. Women who are pregnant should be screened for GBS between weeks 35 and 37 of pregnancy. During delivery, GBS can be transmitted to the baby. In many cases, the baby experiences no symptoms, however they are more at risk for conditions like meningitis and sepsis.
Gram-Negative Bacilli
Gram-negative bacilli includes bacteria like Escherichia coli (E. coli) and Klebsiella pneumoniae. E. coli is a bacteria commonly spread through contaminated food products. You may recall numerous human and pet food recalls in recent years due to E. coli contamination. Mothers can transmit Gram-negative bacilli during birth.
Listeria Monocytogenes
Baby’s can get listeria from their mother while still in the womb. If a mother eats something that is contaminated with listeria, it can enter her bloodstream and be passed along to the baby.
Since the virus, bacteria or fungus that causes infant meningitis can be transferred from mother to baby, prenatal care and virus screening for the disease is extremely important. Any of these viruses or bacteria can result in the mother passing an infection to her baby during labor and delivery. Other ways of exposure include coming into contact with anyone who carries the virus, such as kissing someone who is infected. Casual contact, such as holding an infant, doesn’t usually result in exposure.
Fungal Causes
Fungal meningitis is more rare than viral or bacterial. Babies most at risk for fungal meningitis are those with weak immune systems. Still, it is important to be aware of fungal causes of meningitis.
Candida
Babies born prematurely are most at risk from the fungus Candida. Candida is a common fungus that lives in the body and on the skin without causing symptoms. It can also live on surfaces in the hospital. Candida can enter the bloodstream and cause infection (candidiasis), which can then travel to the brain and cause meningitis.
Cryptococcus
Cryptococcus neoformans is a type of fungus that lives in the environment. It is present all over the world. People who come in contact with the microscopic fungus usually never get sick from it. However, people with weak immune systems can develop meningitis.
Histoplasma
Histoplasma is a fungus that lives in the environment, mostly in soil, but is also found in bat and bird feces. The fungus is most common in the central and eastern parts of the United States, Asia, Africa and Australia. The fungus can cause an infection called histoplasmosis. People with weak immune systems can experience severe symptoms, spreading infection and meningitis.
Blastomyces
Blastomyces is a fungus that lives in the environment in soil and decomposing matter like leaves and wood. Breathing in the spores can cause an illness called blastomycosis. Most people never get sick from breathing in the spores. However, some people do develop fever and a cough, which can lead to a more serious infection. Without proper treatment, it can further lead to meningitis.
Coccidioides
This fungus lives in the soil in the southwestern U.S. and parts of North and Central America. Breathing in the microscopic spores can cause an illness called coccidioidomycosis, or valley fever. People who get valley fever are at risk for serious illness, including meningitis.
Symptoms of Meningitis in Babies
Symptoms of meningitis often appear rapidly. At first, most parents only notice tiredness or irritability. But then the symptoms appear quickly and it is important to get your child medical attention right away. If your infant suddenly begins experiencing symptoms, it may be difficult to comfort them. They may be experiencing a variety of symptoms that they can’t tell you about, so it is important to recognize the symptoms and when to get help.
Symptoms of meningitis in babies often include:
- Bulging in the baby’s soft spot, or fontanel (this is due to increased fluid or pressure on the brain)
- Fever (babies under three months may not have a fever. Those over three months may spike a high fever)
- Infants who have a high fever may also experience seizures if they have meningitis
- Dark or red rash marks across the body
- Cold hands and feet but torso is warm
- Neck stiffness (the baby may tilt their head and be stiff in the upper body)
- Nausea or vomiting
- Extreme sleepiness or difficulty waking
- Not being as active as usual
- Being more irritable than usual
- Poor feeding habits
With newborns, many symptoms are difficult to identify, such as headaches or nausea. However, many of the symptoms above can be readily identified by attentive parents or caregivers. It is important that any signs of infection are taken seriously and the baby is assessed by a doctor as soon as possible.

Symptoms of Group B Strep among Mothers
Most mothers do not know that they have Group B Strep. In fact, doctors say that around 40% of women carry Group B Strep in the lower intestines, rectum and vagina without even knowing it. There are no symptoms that indicate that the mother has the bacteria in her system – these women are called asymptomatic carriers. Women who do have symptoms may experience more frequent urinary tract infections (UTIs), blood infections or pneumonia.
By testing anywhere between weeks 35 and 37 of pregnancy, the doctor should be able to identify whether the mother has Group B Strep. During labor and delivery, she will receive pregnancy-friendly antibiotics to help combat the infection and prevent it from spreading to the baby.
Tests to Confirm Meningitis Diagnosis
If you suspect that your child may have meningitis, the best thing you can do is take them to a doctor to confirm your suspicions. To confirm a meningitis diagnosis, your doctor will examine the baby and then run some tests. These tests may include:
- Blood cultures: Blood is taken from the infant and is placed on a plate that grows viruses, bacteria or fungi. If something grows, doctors can tell the cause of meningitis and make an accurate diagnosis.
- Blood tests: Blood can also be analyzed in a lab for signs of infection.
- Spinal tap: A test that removes some fluid from around the spinal cord. It can also be analyzed or subjected to culture tests. Culture tests involve placing the fluid on special plates and then monitoring it to see if anything grows.
- CT scan: Computed tomography (CT scan) can show if there is a pocket (abscess) of infection in the brain.
How is Meningitis Treated?
As mentioned earlier, infant meningitis is a very severe condition, and if you catch any of these signs in your baby, medical treatment is imperative. The type of treatment that your baby needs will depend on the type of meningitis they have, how serious it is and how their general health is. Treatment options may include:
Treating Viral Meningitis
Many babies who develop viral meningitis will get better without treatment. Meningitis that is caused by viruses like enteroviruses or influenza often clears up within 10 days without requiring treatment. Other viruses like varicella or HSV are more serious, and your baby may need to be treated with intravenous (IV) antiviral medication. Sometimes this requires hospitalization to monitor the baby during treatment.
Treating Bacterial Meningitis
Bacterial infections generally do not clear up on their own like viral infections. Therefore, cases of bacterial meningitis often require IV antibiotics. Most likely, your baby will stay in the hospital while receiving the medication. Doctors and nurses will closely monitor your baby to make sure the treatment is working.
If meningitis isn’t treated immediately, the bacteria can affect the brain causing potential brain damage and death. If brain damage occurs, the infant may develop cerebral palsy. Cerebral palsy is a motor disorder caused by brain damage. It causes difficulties with mobility, motor skills, communication and more.
Treating Fungal Meningitis
Fungal infections can be severe and often take a long time to clear up. Most people who have fungal meningitis – regardless of age – will be treated with IV antifungal medications. Many people stay in the hospital for up to a month while the fungal infection clears up.
Can Meningitis be Prevented?
Because there are various types of infections that can cause infant meningitis, it is difficult to say what could possibly prevent it. However, there are some things that mothers and healthcare providers can do. For example, recognizing the illnesses that most commonly cause meningitis in infants and children. As noted above, there are many possible illnesses and bacteria that can lead to meningitis. There are three, however, that are most common in infants over one month old and children under five years old. These are:
Streptococcus Pneumoniae
Bacterium is present in the sinuses and lungs. If someone who is infected coughs or sneezes, those nearby can inhale the germs into their lungs. This is the most common cause of bacterial meningitis in children under two years old.
Neisseria meningitidis
This is the next most common cause of bacterial meningitis in babies under one year old. It also spreads via oral secretions, particularly breathing in a cough or sneeze from someone infected. Babies can also be exposed through sputum if someone is in their face or kissing them.
Haemophilus influenzatybe b (Hib)
Hib carriers generally do not have symptoms, but they can spread Hib via oral secretions, such as kissing the baby. In most cases, a baby would have to be in close contact for a few days or longer in order to be exposed. A vaccine (Hib) has caused haemophilus type B meningitis to become extremely rare. Unfortunately, the vaccines that do exist to prevent meningitis are most often only available to older children and adults.
Having your child vaccinated against these illnesses is the key to preventing meningitis. Vaccines like Hib and pneumococcal help protect babies from the bacteria and viruses that commonly cause infections and meningitis.
How Parents Can Help
In addition to vaccines, there are some things that parents and caregivers can do to help prevent meningitis and other illnesses that may affect babies. These include:
- Make sure anyone with a cold sore does not kiss a newborn baby.
- Keep newborns away from anyone who is sick, sneezing, coughing or who has a fever.
- Keep newborns out of large crowds.
- Wash your hands thoroughly before preparing baby bottles, formula or food.
- Ask visitors to wash their hands before touching or holding your baby.
- If you are pregnant, make sure your doctor does a Group B strep test between 35-37 weeks.
- If you are positive for Group B strep, you should be given antibiotics during labor.
- When it is prime mosquito season, protect your baby as much as possible. Keep them inside when mosquitos are out, or put them in pants and long sleeves.
- Ask your pediatrician for recommendations on safe and effective bug repellant.
- Do not expose your baby to cigarette smoke.
Prognosis for Meningitis
If infant meningitis is diagnosed and treated quickly, the prognosis is generally favorable. Most infants fully recover as long as they get adequate treatment. According to the Centers for Disease Control and Prevention (CDC), around 80-90 percent of people who develop meningitis caused by meningococcal bacteria survive. If treatment is delayed, however, the prognosis is not as good. Delayed treatment can result in long-term effects, such as:
- Blindness
- Deafness
- Seizures
- Hydrocephalus
- Brain damage
The CDC estimates that between 11 and 19% of children with meningococcal bacteria infections experience long-term effects. Ultimately, immediate diagnosis and treatment is the best way to improve your child’s prognosis and get the best outcome.
Start Your FREE Case Review Today
If you or your child is injured as a result of medical negligence, call us to learn more.



